Joint Pain vs Tendon Pain: A Complete Guide to Understanding the Difference
If you’ve ever experienced pain in your shoulder, knee, or elbow, you’ve probably wondered whether the problem lies in the joint itself or the surrounding tendons.
“So, Basically you faced joint pain or tendon pain confuse will be go out shortly“
While these two types of pain can feel similar and often occur in the same areas, they’re fundamentally different conditions that require different approaches to treatment. Understanding the distinction can help you get the right care faster and avoid complications down the line.
What’s the Real Difference Joint Pain vs Tendon Pain?
Joint pain originates from within the joint structure itself—the space where two or more bones meet. This includes the cartilage, synovial fluid, joint capsule, and the bone surfaces. Think of conditions like arthritis, where the protective cartilage wears down, or when inflammation builds up in the joint space.
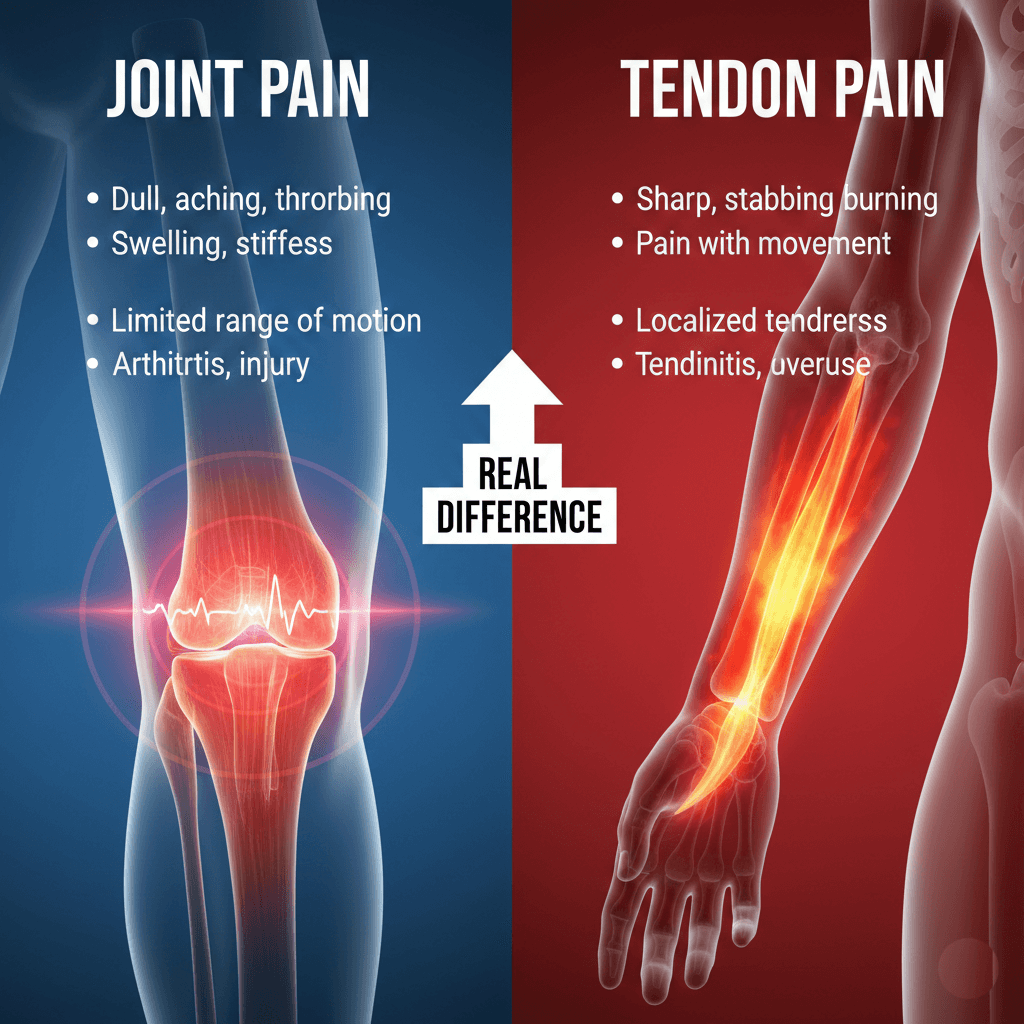
Tendon pain, on the other hand, affects the tough, fibrous cords that connect muscles to bones. When these structures become inflamed or irritated—a condition we call tendinitis or tendinopathy—the pain you feel comes from the tendon tissue itself, not the joint. Common examples include tennis elbow, Achilles tendinitis, or rotator cuff tendinopathy.
How to Tell Them Apart
The location of your pain provides the first clue. Joint pain typically feels deep within the affected area—inside your knee, deep in your hip, or centrally located in your shoulder.
You might describe it as an ache that seems to come from “inside” the joint. Tendon pain, conversely, tends to be more superficial and localized. You can often pinpoint it to a specific spot along the tendon’s path, like the outside of your elbow or just above your heel.
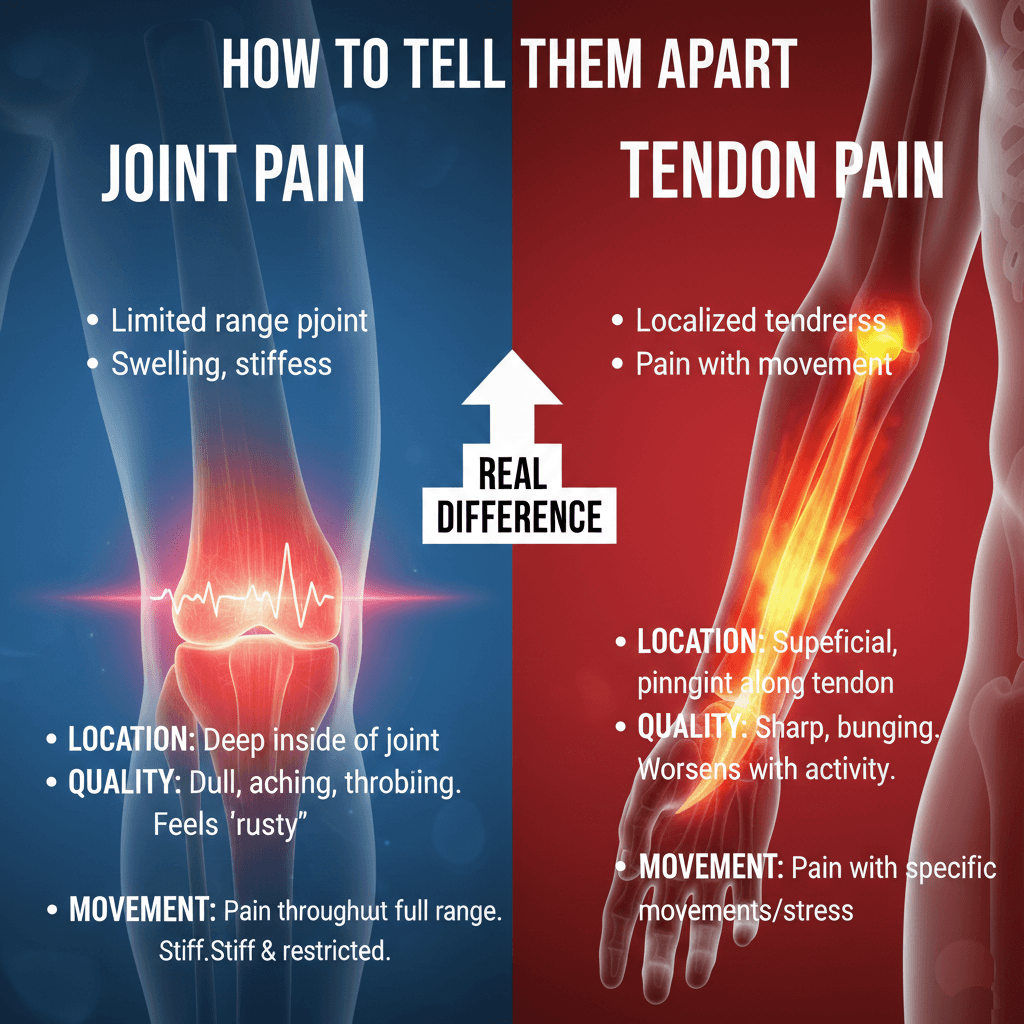
The quality of pain differs too. Joint pain often presents as a constant, dull ache that may throb or feel stiff, especially after periods of rest.
Many of my patients describe their arthritic joints as feeling “rusty” first thing in the morning. Tendon pain is usually sharp and may feel like a burning or stinging sensation, particularly during movement. It often starts gradually and worsens with specific activities that stress the affected tendon.
Movement patterns tell an important story. With joint problems, you’ll typically notice pain throughout the entire range of motion, and the joint might feel stiff or restricted in multiple directions.
Your knee might hurt whether you’re bending it, straightening it, or putting weight on it. Tendon pain is more selective—it hurts with specific movements that load or stretch the tendon but may feel fine with other motions. For instance, someone with Achilles tendinitis might struggle with rising onto their toes but feel okay walking on flat ground.
Common Causes and Risk Factors
Joint pain frequently stems from degenerative changes like osteoarthritis, where years of wear and tear break down cartilage. Inflammatory conditions such as rheumatoid arthritis, gout, or lupus can also target joints.
| Category | Cause | Explanation |
|---|---|---|
| Joint Issues | Acute Injuries | Sprains, dislocations, or fractures that extend into the joint surface can damage joint structure and cause pain. |
| Joint Issues | Age-Related Degeneration | Most people over 60 show some degree of joint degeneration, even if they do not experience symptoms. |
| Tendon Issues | Overuse or Repetitive Stress | Repeated strain from physical activity can gradually irritate or damage tendons. |
| Tendon Issues | Physically Demanding Activities | Athletes and individuals with labor-intensive jobs are more vulnerable to tendon pain. |
| Tendon Issues | Poor Biomechanics | Improper running form or incorrect lifting techniques can overload tendons over time. |
| Tendon Issues | Tendon Degeneration | Tendons may lose resilience with age, becoming more prone to injury, especially in middle age. |
| Tendon Issues | Sudden Increase in Activity | Rapid shifts from low activity to intense exercise (common in “weekend warriors”) often trigger tendon problems. |
Sometimes tendons degenerate over time, becoming less resilient and more prone to injury—this is especially common in middle age. Sudden increases in activity levels often trigger tendon problems; weekend warriors who go from sedentary to highly active are classic examples.
What You Might Notice
Beyond the pain itself, joint and tendon problems have distinct associated symptoms. Joints affected by inflammatory arthritis often swell visibly, may feel warm to the touch, and can appear red. You might hear or feel grinding, clicking, or popping sounds—what we call crepitus. Many people notice their joints are particularly stiff after waking up or sitting for long periods, and this stiffness can last anywhere from a few minutes to over an hour with inflammatory conditions.
Tendons typically show localized swelling along the tendon’s course rather than diffuse joint swelling. The area may be tender to touch, and you might feel a thickening or a nodule on the tendon itself. Unlike joint stiffness that improves with gentle movement, tendon pain often worsens as you continue the aggravating activity. Some people notice their affected tendon feels “creaky” or makes a crackling sensation when they move it.
Getting the Right Diagnosis
While being aware of these differences helps, proper diagnosis requires professional evaluation. I always start with a detailed history and physical examination.
For joint problems, I’m looking at range of motion, stability, swelling patterns, and specific tests that stress the joint structures.
X-rays can reveal arthritis, fractures, or joint space narrowing, while MRI scans provide detailed images of cartilage, ligaments, and the joint capsule. Blood tests might be necessary if I suspect inflammatory arthritis.
Evaluating tendon pain involves palpating along the tendon’s length, testing strength with resistance, and performing specific maneuvers that reproduce the pain.
Ultrasound is excellent for visualizing tendons—it’s dynamic, meaning I can watch the tendon move in real-time, and it’s particularly good at showing inflammation, tears, or degeneration.
MRI also works well for tendons, especially when I need to see surrounding structures or rule out other problems.
Treatment Approaches
The good news is that both conditions respond to treatment, though the strategies differ. For joint pain, the focus is on reducing inflammation, protecting remaining cartilage, and maintaining function. You can take JOINTGENESIS for treatment
This might include anti-inflammatory medications, physical therapy to strengthen supporting muscles, weight management to reduce joint stress, and sometimes injections of corticosteroids or hyaluronic acid. In severe cases, joint replacement surgery can be life-changing.
Tendon pain requires patience—tendons heal slowly because they have limited blood supply. The cornerstone of treatment is modifying or temporarily avoiding the activities that caused the problem.
Physical therapy emphasizing eccentric exercises (where the muscle lengthens while contracting) has strong evidence for effectiveness.
Ice can help in the acute phase, while other modalities like therapeutic ultrasound or shock wave therapy may be beneficial for chronic cases. Surgery is rarely needed but might be considered for severe tears or when conservative treatment fails.
The Bottom Line
While joint pain and tendon pain can coexist and sometimes complicate each other, recognizing the differences helps you communicate more effectively with your healthcare provider and understand your treatment plan.
Joint pain typically feels deep, affects multiple movement directions, and often involves visible swelling or warmth. Tendon pain is more localized, hurts with specific motions, and usually develops from overuse.
Neither condition should be ignored. Early intervention, especially for tendon problems, can prevent acute issues from becoming chronic ones. If you’re experiencing persistent pain in any area, whether you think it’s joint or tendon-related, getting it properly evaluated is the first step toward feeling better and returning to the activities you enjoy.





One Comment
Comments are closed.